Clinical documentation has long been one of the biggest sources of burnout in healthcare. Studies consistently show that physicians spend roughly two hours on paperwork for every one hour of direct patient care. AI clinical documentation tools aim to change that by listening to patient encounters and automatically generating structured, EMR-ready notes.
The market has matured rapidly. In 2026 there are more options than ever, each with different strengths. Below we break down the seven tools worth evaluating, what sets them apart, and what to consider when choosing one for your practice.
What to look for in an AI documentation tool
Before diving into specific products, here are the criteria we used to evaluate each tool:
- Accuracy — How reliably does it capture medical terminology, drug names, and clinical nuance?
- Note customization — Can you configure note templates to match your specialty and workflow?
- Platform support — Does it work across the devices you already use (desktop, mobile, wearables)?
- Security and compliance — Is it HIPAA-compliant with end-to-end encryption?
- Pricing — Is the cost reasonable relative to the time you save?
- EHR integration — Can notes be exported or pushed directly into your electronic health record?
1. Medical Scribe
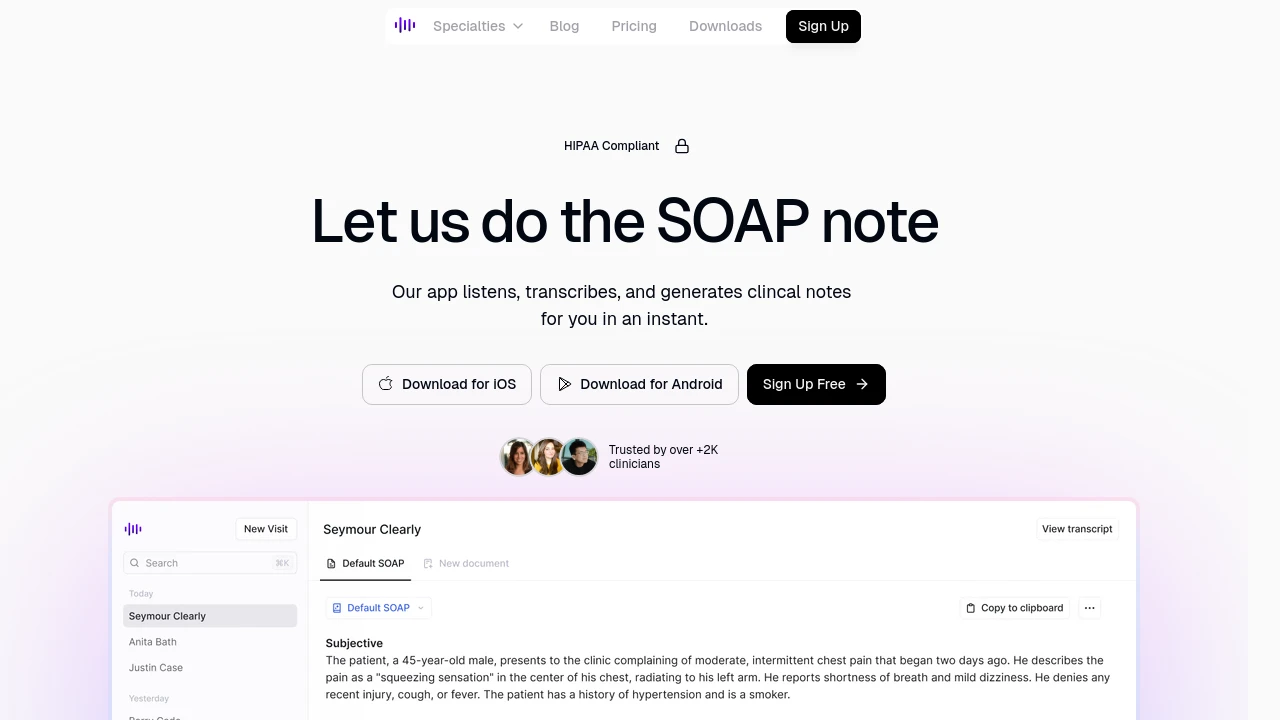
Medical Scribe is the fastest and most adaptable AI scribe available today. It works natively on iPhone, Apple Watch, Mac, and the web, letting you record patient consultations from any device and receive a completed SOAP note in seconds.
Highlights:
- Speech-to-text models purpose-built for medical terminology, supporting 57 languages
- Fully customizable note templates for any specialty
- Apple Watch companion for hands-free recording during procedures
- HIPAA-compliant with AES-256 encryption at rest and TLS in transit
- Free tier available; Pro plan starts at $99/month per provider
Medical Scribe stands out for its speed and flexibility. Whether you are in family medicine, cardiology, or acupuncture, the note output adapts to your preferred structure with minimal setup.
2. Nuance DAX Copilot
Microsoft’s Nuance DAX Copilot leverages the company’s deep investment in ambient AI and its integration with the Microsoft ecosystem. It listens to patient-clinician conversations and drafts notes directly inside supported EHR systems.
Highlights:
- Deep Epic and other major EHR integrations
- Ambient listening with automatic note generation
- Backed by Microsoft’s enterprise security infrastructure
- Best suited for large health systems already on the Microsoft stack
DAX Copilot is a strong choice for organizations that want a tightly integrated enterprise solution, though it can be complex to deploy and is priced at the higher end of the market.
3. Abridge
Abridge has gained traction for its conversational AI that generates structured clinical notes while providing real-time linked evidence. It is designed for health systems and has partnerships with several major hospital networks.
Highlights:
- Real-time note generation with linked evidence from the conversation
- Strong EHR partnerships (Epic integration)
- Designed for multi-specialty health systems
- Focus on transparency — clinicians can trace every note sentence back to the conversation
Abridge is a good option for organizations that prioritize auditability and want clinicians to easily verify AI-generated output.
4. Suki
Suki positions itself as a voice-powered AI assistant that goes beyond documentation. In addition to generating notes, it can help with diagnosis coding and order entry through voice commands.
Highlights:
- Voice-first interface for note creation and clinical workflows
- ICD-10 and CPT coding assistance
- Integrations with several major EHRs
- Specialty-specific vocabulary packs
Suki works well for clinicians who want a single voice interface that handles both documentation and administrative tasks like coding.
5. DeepScribe
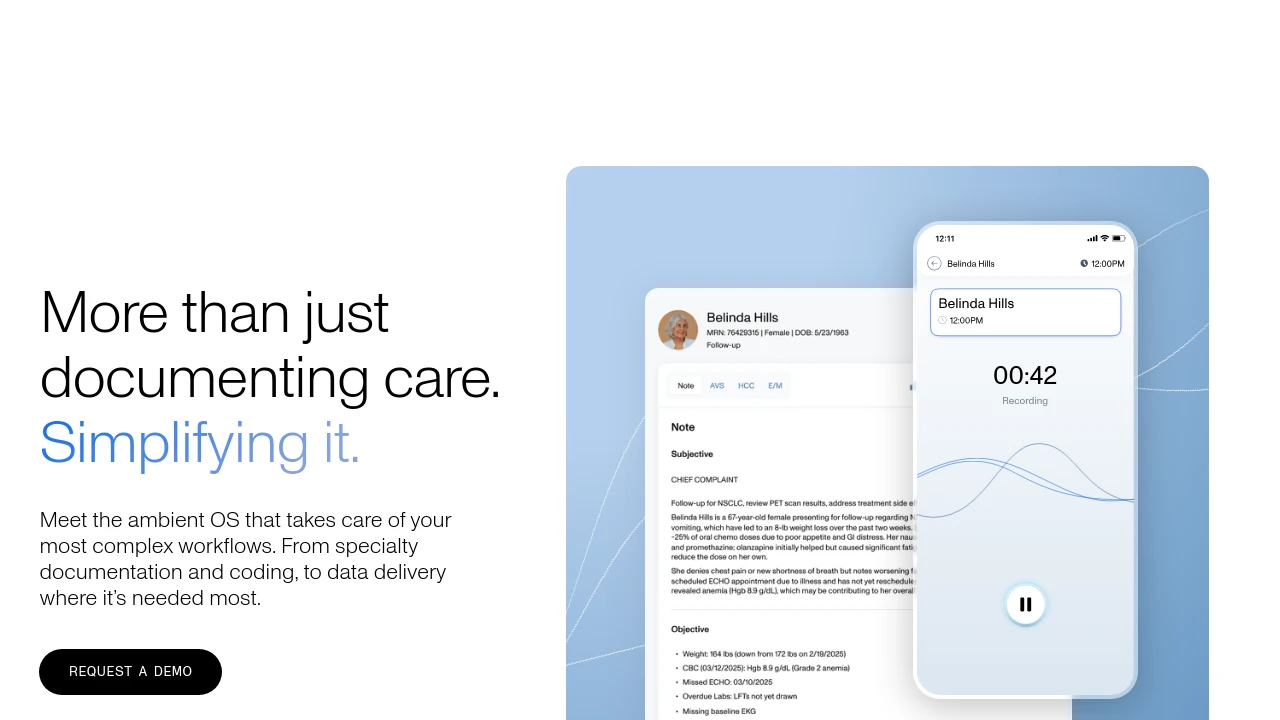
DeepScribe uses ambient AI to document patient encounters and has focused on serving specialty practices. Its models are trained to handle the unique terminology and workflows of various medical disciplines.
Highlights:
- Specialty-trained ambient documentation
- Customizable note templates by specialty
- Direct EHR integration
- Quality assurance review layer
DeepScribe is worth considering if you are in a specialty that requires highly specific documentation patterns and want a tool tuned for that context.
6. Freed
Freed is a newer entrant that has gained attention for its simple interface and fast setup. It is designed for independent practices and small clinics that want AI documentation without a lengthy onboarding process.
Highlights:
- Minimal setup — start documenting in minutes
- Affordable pricing for solo and small-group practices
- SOAP, H&P, and custom note formats
- Web and mobile support
Freed is a solid choice for providers who want to get started quickly without enterprise-level complexity.
7. Heidi Health
Heidi Health offers AI-powered clinical documentation with a focus on the global market, supporting multiple languages and healthcare systems. It provides both real-time transcription and note generation.
Highlights:
- Multi-language support for international practices
- Real-time transcription with structured note output
- Templates for a wide range of specialties
- Free tier available with paid plans for advanced features
Heidi is a good fit for practices outside the United States or multilingual clinical settings that need documentation support across languages.
How to choose the right tool
The best tool depends on your practice size, specialty, device preferences, and budget. Here is a quick framework:
- Solo or small practice on Apple devices — Medical Scribe offers the fastest path to time savings with native iOS, watchOS, and Mac apps, plus a free tier to start.
- Large health system on Epic — DAX Copilot or Abridge provide deep EHR integration at enterprise scale.
- Voice-first workflow — Suki combines documentation with coding and order entry in a single voice interface.
- Specialty-heavy practice — DeepScribe and Medical Scribe both offer strong specialty customization.
- Quick start, minimal budget — Freed and Medical Scribe’s free tier let you get up and running immediately.
The bottom line
AI clinical documentation tools are no longer experimental. They reliably save clinicians 30 to 60 minutes per day, reduce after-hours charting, and help combat the documentation burden that drives burnout. The key is finding the tool that fits your workflow, integrates with your systems, and earns your trust through accurate, customizable output.
If you are evaluating options, we recommend starting with a free trial. Medical Scribe offers a free tier with no credit card required — record a patient visit on your iPhone or Mac and see the SOAP note generated in seconds.

